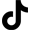Eyelid Skin Cancer Excision
Before and After Photo Gallery
-
 Patient Seeing Straight
Patient Seeing Straight
-
 Patient Seeing Side
Patient Seeing Side
-
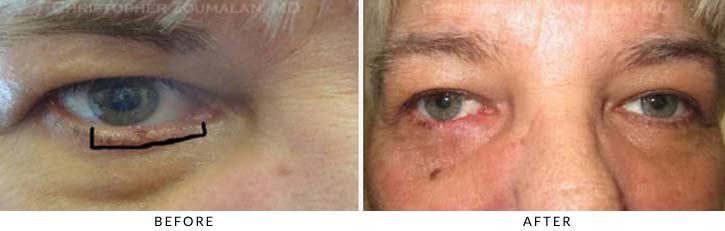
This patient had a large left lower lid skin cancer (basal cell carcinoma). Mohs surgery by a dermatologist was performed to remove the skin cancer (which is located between the black border as shown above). The patient had over 33% loss of his lower lid from the Mohs surgery. Dr. Zoumalan performed eyelid reconstructive surgery to help repair the defect. A skin/muscle advancement flap was used to repair the defect. The post operative photos were taken 3 months after surgery. Notice the natural looking result and normal lid position and contour.
-
Patient Seeing Straight
-
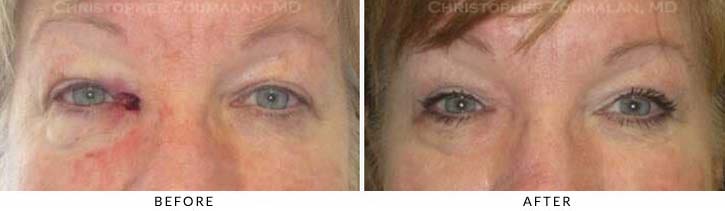
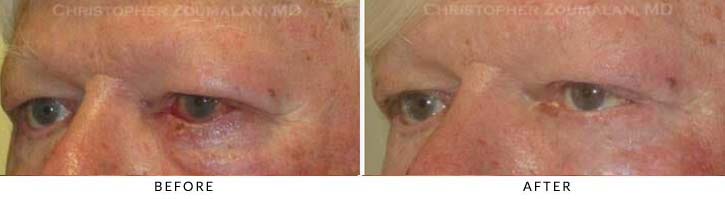
This patient had a biopsy proven right medial canthal (eyelid) basal cell skin cancer. It was removed by a Mohs trained dermatologist. The skin cancer also involved her tear duct system. Dr. Zoumalan was able to reconstruct her defect using local skin flaps. Her tear duct was also reconstructed with the use of silicone tubes as stents. Her post operative photograph was taken six months after surgery and note the natural appearing result with very well healed incisions. Her tear duct system remains patent and functioning normally.
-
Patient Seeing Side
-
This patient was diagnosed with an atypical pigmented lesion (pre-melanoma) in her right lower lid. Treatment required complete excision with several millimeters of free margin tissue. She underwent excision of the lesion and eyelid reconstruction was then performed. A local skin muscle flap was used to fill in the defect. The procedure is also referred to as a Tenzelmyocutaneousreconstructive flap.
-
Patient Seeing Straight
-
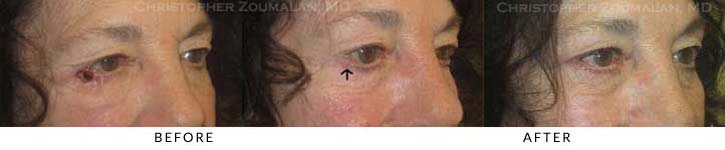
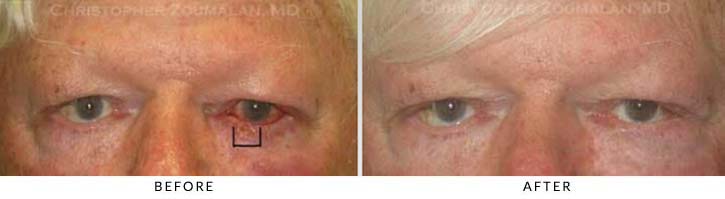
1) This patient had a recurrent squamous cell carcinoma of the left eyelid. It involved the medial (closest to the nose) portion of his upper and lower eyelid.
2) The surgical plan was to have the patient undergo a Mohs excision of the tumor by a Mohs-trained Dermatologist. The black outline depicts the area of resection that was necessary in order to clear the tumor and have clear (tumor-free) margins.
3) This photograph (top right) was taken 6 monts after surgical repair. The patient had siginficant loss of tissue in the medial aspect of his eyelids and had to undergo two local skin and muscle advancement flaps to mobilize local tissue to close the defect. He also lost his tear ducts during the removal of the tumor but has since remained tumor free and very happy with the cosmetic results.
If it is a small defect, often local tissue can be rearranged or brought together to repair the eyelid. If it is a large defect like seen in the photo below, up to 80 percent of the lower lid is mssing along with the tear duct system. In such instances, tissue from the upper lid is often needed to repair the defect through a procedure called a Hughes flap (aka tarsoconjunctival flap) named after one of the pioneers in Oculoplastic Surgery, Dr. Wendell Hughes. Tissue is taken from the upper lid as seen in this following photo and transfered in the lower lid. Unfortunately, the eyelid is sewn shut for at least one month until the flap takes place. A second surgery is then performed to “take down” the flap and allow for the eyelid to be reconstructed to a normal-appearing eyelid.
-
Patient Seeing Straight
-
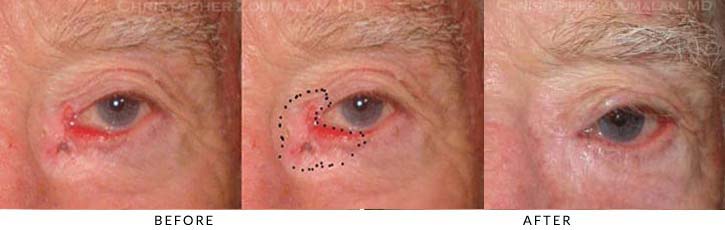
1) This photo above shows a squamous cell carcinoma of the right lower lid that after its complete excision, was left with a defect that spanned the markings drawn on the photo. The resection also involved her lower lid tear duct system. This particular patient did very well after the first stage and went home the same day with little discomfort.
2) The patient underwent a a second stage surgery which was performed several weeks later to detach the flap and reconstruct both upper and lower lids to position them as close to their natural, presurgcial position as possible. She is cancer free, can see from that eye now (top right), and has a good position and contour of her lower lid. Note that she has lost her eyelashes in the lower lid which occured once the tumor was removed in the primary excision.
-
Patient Seeing Side
-
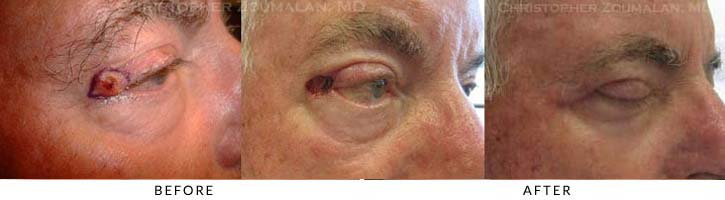
1) This patient presented with a squamous cell carcinoma of his right upper lid (Top left photo). Marking pen was drawn around the lesion prior to it being excised.
2) Once the biopsy was proven to be a malignancy, MOHS surgery was then performed by a fellowship-trained MOHS surgeon to completely remove the lesion and to provide free margins of healthy tissue. (Middle photo).
3) Next, the defect was repaired by Dr. Zoumalan using local tissue advancement flaps once the MOHS surgeon had completed the resection. This picture was taken a little over three weeks after surgery.
Disclaimer:
*Individual results may vary
All before and after pictures displayed are real patients who have consented to having their pictures published on our site. Individual results will vary with each patient and Dr. Christopher Zoumalan does not guarantee any outcomes of procedures shown. All pictures are meant for reference and illustrative purposes only.